Personalizing the pediatric perioperative patient experience
When 70% of your patients are younger than ten years old, and 75% of them experience preoperative anxiety, you need to get creative about personalizing patient experiences to ease fears—especially for children with special needs.
So that’s just what Dayton Children’s Hospital leaders accomplished in their perioperative environments, by developing sensory-friendly environments to aid in individualizing their patient experience for children. They also expanded their patient preferences to record how each child is unique—building a nearly instant repertoire with patients by asking them questions about topics such as likes and dislikes, care preferences, and favorite toys, games, or comfort items.
“If they have a history of anxiety, developmental delays, or prior medical visits, each time they come through our doors, there’s a little bit of medical PTSD,” says Sean Antosh, MD, Anesthesia Clinical Director of Special Needs Patient Experience at Dayton Children’s Hospital, at the recent 2024 NRC Health Pediatric Collaborative. “It causes emotional dissatisfaction. As patients come over and over, if we’re doing something they perceive as harmful, their anxieties increase and their outcomes worsen”
Check out the full presentation from the 2024 Pediatric Collaborative.

The power of human-centered design
Several years ago, Dayton Children’s Hospital started a multidisciplinary perioperative patient-experience committee, representing every location a patient goes to.
They measure NRC scores, gather patient and family comments and updates from each area and host a round table of ideas and process improvements. From that committee, they realized they didn’t have a good way of telling families what to expect from a visit to the hospital.
Research shows that cartoons are one of the best ways to do this—even better than live-action videos—and help the parent more than the child. So at the height of COVID, they spent countless hours developing a video to give families an idea of what to expect.
“Patients and families know exactly what they’re going to see, what they’re going to do,” Antosh says. “That’s just the first step in helping to prepare them and decrease some of that anxiety.
“We have special markers that we purchase that we use to write their name on their bed, and often we’ll draw a picture—and it’s usually in black and white, so they have the opportunity to come in and continue to color on their bed and color in the picture that we’ve drawn.
“This allows them to feel a little bit of control over their environment. And any piece of control you can give a kiddo, the better they’ll feel about the whole situation in general, because this is a situation, coming for surgery, where they feel very much not in control. And it’s also a way for us as Child Life specialists and staff members to get a glimpse of what’s going on in their brain. It gives us a clue that we can use to build rapport with those patients and families.”
Antosh explains that as Child Life specialists, they know that unexpected stress is more traumatic—so Dayton Children’s gives patients the mask they’ll use when they’re anesthetized ahead of time, and allows them to choose six stickers to customize it.
“These kids are in a stage of development where they really benefit from freedom within limits and being given opportunities for control,” Antosh says. “So choosing from stickers and special oils to make [the mask] smell delicious allows them to control and personalize their experience and gives them power over the situation. During that time, we also show them photos of the OR, so they know exactly where they’re going to go, what their job is, what their role is, who’s going to be in the room, and what the room will look like when they wake up, with actual photos. It’s been super, super helpful for those kids.”
Results to improve care delivery
Since implementing things like the bed areas, customized masks, and the patient’s choice of how they go to the OR (in Tyke Cars, little airplanes, or princess carriages), providers have recorded that median recovery time has decreased from 37 minutes to 32 minutes.
“When we started this work, we just looked at the comments—we didn’t care about the scores,” Antosh says. “We’re very proud of making sure we try to hit that mark every time.”
Dayton Children’s providers have also taken great strides in using innovative sensory tools to humanize pediatric surgery by creating Adaptive Sensory Environments (ASEs), which have been especially helpful for neurodiverse patients.
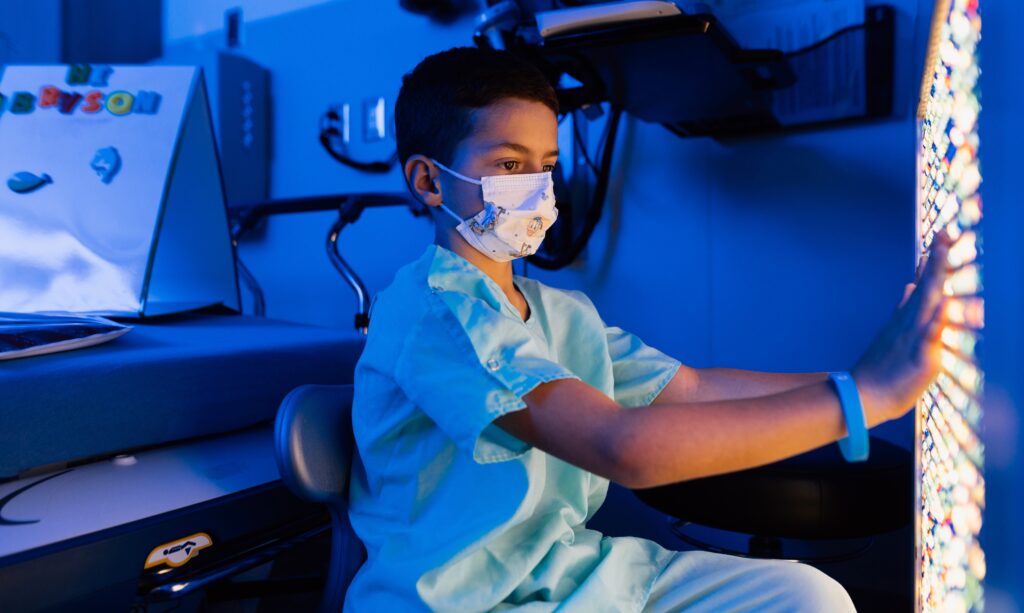
What is an ASE?
- An immersive sensory space for individual patients to interact with and enjoy sensory experiences
- A safe, relaxing space that allows for de-escalation from sensory overload or feeling overwhelmed, anxious, and/or hyperactive.
- A space specifically tailored for the patient, based on their individual coping plan regarding hyper/hypo – responsiveness to sensory stimuli
Dayton Children’s combined research, innovation, and education to form a culture change for patient experience and introduce their Penguin Patients program to those who need a different perioperative process. This program includes early identification and contact, development of and easy access to individualized coping plans by Child Life specialists, flexible admission processes and decreased wait times, adaptive sensory environments, and education for perioperative nursing and anesthesia staff.
The coping plan covers triggers that easily upset a child, signs that a child is distressed, the best ways to comfort them or help them relax, advice on what to do if a procedure isn’t going well, any environmental accommodations needed, patient interests and past medical experiences, and specifics on autism or any other developmental delay relevant to the patient.
“The coping plan started just for kids who had developmental delays, autism, Down syndrome, CP, and things like that,” says Katelyn Shellabarger, CCLS, Certified Child Life Specialist at Dayton Children’s Hospital. “And it’s opened up more towards kids who also are chronic patients, who are here all the time, or kids who are just super anxious about pokes, about IVs, about lab draws, about the hospital in general.”
The results? The median recovery time for patients with Autism Spectrum Disorder requiring premedication decreased, and there was an increase in the number of patients not requiring either Midazolam or ketamine. The median recovery time was also reduced by nine minutes.
“We found that while we still have to give these medications, the patients are so much calmer when we’re trying to get the medications in them,” Shellabarger says. “Truly, I could cry just recalling a comment that said, ‘My child was not treated as a number or as a patient or a number—was treated as the small feeling human that she is. Thank you from the bottom of my heart for the concept of this flawless execution.’”
Click here to view the entire presentation from the NRC Health 2024 Pediatric Conference.


